I discuss issues pertaining to the practice of neuropathology -- including nervous system tumors, neuroanatomy, neurodegenerative disease, muscle and nerve disorders, ophthalmologic pathology, neuro trivia, neuropathology gossip, job listings and anything else that might be of interest to a blue-collar neuropathologist.
Wednesday, May 30, 2018
Moving beyond histologic grading of IDH-wildtype diffuse astrocytic gliomas
Despite the fact that the most recent update of the World Health Organization (WHO) classification of central
nervous system tumors was published only two years ago, the data is already showing that we are moving beyond that classification system when if comes to IDH-wildtype diffuse astrocytomas. The concept of an "integrated diagnosis" in the setting of IDH-wildtype histologic grade II and III tumors has already been eclipsed in the literature by the primacy of the genetic signature over histologic appearance in predicting outcome. In the near future, diffuse IDH-wildtype astrocytic gliomas with (1) combined whole chromosome gain of 7 and loss of 10, and/or (2) EGFR amplification will be designated as equivalent to WHO grade IV gliomas. Histologic grades for such tumors will be stricken from the top diagnostic line so as to avoid unfounded reassurance that these tumors will behave in any way other than very aggressively.
Friday, May 25, 2018
Dr. Dan Brat interviewed on Northwestern Feinberg School of Medicine Podcast
In the latest episode of the Northwestern Medicine Breakthroughs podcast, Daniel Brat, MD, PhD discusses the emerging integrated molecular-histomorphological classification of diffuse gliomas. In an episode entitled "A New Way to Diagnose Brain Tumors", Dr. Brat -- the new chairman of the Northwestern Pathology -- states that "whenever you go through a reclassification that dramatic, there's going to be gaps in knowledge and gaps in practice and we are recognizing those gaps on a
daily basis, on a yearly basis. And we as a brain tumor community internationally are working to fill those gaps in knowledge. So what we found for example, is that once you classify molecular diseases, the grading criteria that we used in the past to grade things as [World Health Organization] grade one, grade two, grade three, grade four, which really served to predict how patients are going to fair and what type of therapies they are going to need, all of those grading criteria needed to be recalibrated. And that's a significant undertaking as well. And we have certain initiatives within the international community through an organization called cIMPACT-Now [Consortium to Inform Molecular and Practical
Approaches to CNS Tumor Taxonomy – Not Official WHO]. And we as a group, including some colleagues here at Northwestern Feinberg School of Medicine, are writing the guidelines for new grading criteria for the diffuse gliomas within the molecular era." . The podcast aired on May 15 and is available on iTunes and SoundClound.
 |
| Dr. Dan Brat |
Thursday, May 24, 2018
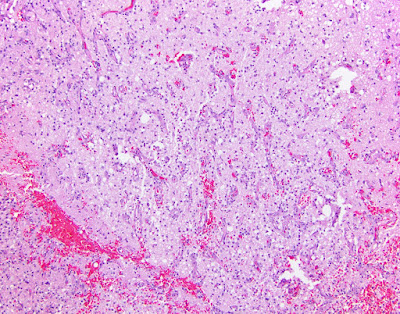
Best Post of April 2018: Exuberant endothelial reactive hyperplasia next to a subacute infarct biopsied to rule out neoplasia
The next is on "Best of the Month" series is from Tuesday, April 3, 2018:
Tuesday, May 22, 2018
The "specific glioneuronal element" of dysembryoplastic neuroepithelial tumor
 |
| A "floating neuron" is circled in this "specific glioneuronal element" of a DNT |
Thursday, May 17, 2018
Astroblastoma
This is a rare, as yet ungraded, cerebral tumor of childhood. It is composed of cells that are GFAP positive and have broad, non-tapering processes radiating toward central blood vessels (astroblastic pseudorosettes). The border with adjacent brain is pushing, not infiltrative. Hyalinized vessels (as seen below) are a hallmark of astroblastoma. No ependymal features have been identified in studies of this unusual entity.
Wednesday, May 16, 2018
Age of First Football Tackles Tied to Neurobehavioral Symptom Onset
Younger age of exposure to tackle football predicts earlier neurobehavioral symptom onset among players with chronic traumatic encephalopathy (CTE), according to a study recently published online in the Annals of Neurology.
Michael L. Alosco, Ph.D., from Boston University, and colleagues examined the brains of 246 tackle football players donated for neuropathological examination. Of the 211 who were diagnosed with CTE, 126 were without comorbid neurodegenerative diseases. Age of first exposure and age of cognitive and behavioral/mood symptom onset were determined through informant interviews.
Monday, May 14, 2018
Understanding Neurophobia Among Medical and Other Health Care Students
 |
| Andre Toulouse, PhD, (University College, Cork, Ireland) lead author on article about neurophobia |
Reference: Javaid MA, Chakraborty S, Cryan JF, Schellekens H, Toulouse A. Understanding neurophobia: reasons behind impaired understanding and learning of neuroanatomy in cross-disciplinary healthcare students. Anat Sci Educ 11:81-93 (2018).
Thursday, May 10, 2018
Best Post of March 2018 - Featured Neuropathologist: Michael Punsoni, MD
The next in our "Best of the Month" series is from March 12, 2018
 On occasion, we profile a prominent or rising neuropathologist. In the past, we've featured the likes of Craig Horbinski, Roger McLendon, Jan Leestma, and Karra Jones. Today we feature Michael Punsoni, MD, a 2016 graduate of the Brown University Neuropathology Fellowship Program and now on faculty at the University of Nebraska in Omaha. Dr. Punsoni agreed to engage in a little Q&A:
On occasion, we profile a prominent or rising neuropathologist. In the past, we've featured the likes of Craig Horbinski, Roger McLendon, Jan Leestma, and Karra Jones. Today we feature Michael Punsoni, MD, a 2016 graduate of the Brown University Neuropathology Fellowship Program and now on faculty at the University of Nebraska in Omaha. Dr. Punsoni agreed to engage in a little Q&A:
1. Why did you decide to become a neuropathologist?
I have always had a strong interest in science and medicine, particularly the neurosciences. After college I worked in two research labs, which fueled my interest in basic neuroscience but also drove me to pursue a medical degree. During my clinical years of medical school I had a strong interest in neurology but my eagerness to be involved in all facets of medical care led me to apply for a categorical residency in Internal Medicine. While I am grateful for the skills and knowledge I acquired during my medicine internship I came to the realization (on one of my 36-hour calls if I remember correctly) that clinical medicine was not for me. I went back to the specialty drawing board and ultimately found pathology somewhat by chance. One of my patients on the medical floor needed an aspiration biopsy of a neck mass. I met the cytopathologist and watched closely as she aspirated a small amount of material and looked on in awe at the squamous cell carcinoma cells on her bedside dual-head scope. I fell for pathology hard after that and, while re-applying to the match, I went back to what I knew best, another year of neuroscience research. By the time I was in pathology residency, my interest for neuropathology was cemented and there was no going back.
2. What do you like to do outside of work?
Watching old and new movies and finding great hole-in-the-wall type restaurants. I’m always looking for/open to suggestions for either one.
Watching old and new movies and finding great hole-in-the-wall type restaurants. I’m always looking for/open to suggestions for either one.
3. Name a couple of important professional mentors. Why were they important to you?
My two PIs at Cornell Medical Center, Joe Pierce and Theresa Milner for the brilliant work they let me participate in, for teaching me to be meticulous in all things particularly bench techniques and for their good humor that stays with me today. To all four neuropathologists at Brown University who shaped the neuropathologist I would become and still hope to be one day. Dr. Suzanne de la Monte to whom I am grateful for her relentless push to make me a good presenter and for sharing her invaluable tips on manuscript writing. Dr. Douglas Anthony whose leadership skills and commitment to the scientific method were inspiring then and now. Dr. Ed Stopa who treats all his fellows like family and never stops guiding them. Dr. John Donahue who taught me that a remarkable memory is only part of what makes a good pathologist and also, that “it’s a tough job but someone’s got to do it!”.
4. What advice would you give to a pathology resident interested in doing a neuropathology fellowship?
Do an elective at your home institution and/or elsewhere. Try it out. It’s a fascinating field and will be for years to come. As I once heard one of my mentors say, we have our own language (when describing the structures of the brain) and we like it that way. Join the group, we’d love to have you.
5. What city (other than Omaha, of course) would you like a future American Association of Neuropathologists meeting to be held and why?
Honolulu. I’ve never been and this would be a great reason to go. Another desirable place would be Boston, which has great restaurants and a good transit system.
Monday, May 7, 2018
The American Association of Neuropathologists Awarded R13 Conference Grant by National Institute on Aging
The American Association of Neuropathologists (AANP) today announced that it has been awarded an R13 Support for Conferences and Scientific Meetings grant through the National Institute on Aging of the National Institutes of Health. This grant will support the 94th Annual Meeting of the AANP in Louisville, KY.
“We are extremely pleased to be recipients of an R13 grant to support dissemination of the critical work completed by our members and featured by our annual meeting,” said Assistant Secretary Treasurer/Chair of the Education Committee, Edward Lee, MD, PhD. “The National Plan to Address Alzheimer’s Disease calls for the prevention and treatment of Alzheimer’s disease and related dementias (ADRD) by 2025. Critical to this goal is the role of neuropathologists in describing the neuropathology associated with ADRD and aging. To this end, the annual AANP meeting provides the most direct means to disseminate the latest developments in ADRD and aging-related neuropathologies.”
The purpose of the R13 grant through the NIA is to support the ADRD and aging components of conferences and scientific meetings, to better disseminate latest developments related to pathologic heterogeneity in dementia and aging. Specific to the AANP, this grant aims to enhance the education of neuropathology trainees about ADRD and aging to attract the next-generation of ADRD neuropathologists. Notably, this grant markedly expands the support available for trainees to attend the annual meeting such that 30 trainees will receive trainee travel awards this year.
This year’s 94th Annual Meeting will kick-off on Thursday, June 7 with the first half of the Special Course: Neuropathology of Aging featuring the following speakers: Elizabeth Mormino, PhD, Stanford University; John Crary, MD, PhD, Icahn School of Medicine at Mount Sinai; Peter Nelson, MD, PhD, University of Kentucky; and Julie Schneider, MD, MS, Rush University Medical Center. The DeArmond Lecture: Dysregulated Metabolism in the Pathogenesis of Alzheimer’s Disease: Type 3 Diabetes will take place on Friday featuring Suzanne de la Monte, MD, MPH, of the Warren Alpert Medical School of Brown University. In addition, multiple platform sessions throughout the meeting will focus on aging and neurodegenerative diseases including sessions on
Alzheimer’s disease, chronic traumatic encephalopathy, frontotemporal lobar degeneration, Lewy body disease and prion disease. Lastly, this year will also include the first-ever Award for Best Neurodegenerative Disease Case Presented at the 2018 Diagnostic Slide Session.
“We are thrilled to be R13 grant recipients,” said current AANP President Elizabeth Cochran, MD. “Thank you to everyone who dedicated time and focus in developing our proposal, and thank you to the National Institute on Aging for their support.”
 |
| Dr. Edward Lee |
The purpose of the R13 grant through the NIA is to support the ADRD and aging components of conferences and scientific meetings, to better disseminate latest developments related to pathologic heterogeneity in dementia and aging. Specific to the AANP, this grant aims to enhance the education of neuropathology trainees about ADRD and aging to attract the next-generation of ADRD neuropathologists. Notably, this grant markedly expands the support available for trainees to attend the annual meeting such that 30 trainees will receive trainee travel awards this year.
This year’s 94th Annual Meeting will kick-off on Thursday, June 7 with the first half of the Special Course: Neuropathology of Aging featuring the following speakers: Elizabeth Mormino, PhD, Stanford University; John Crary, MD, PhD, Icahn School of Medicine at Mount Sinai; Peter Nelson, MD, PhD, University of Kentucky; and Julie Schneider, MD, MS, Rush University Medical Center. The DeArmond Lecture: Dysregulated Metabolism in the Pathogenesis of Alzheimer’s Disease: Type 3 Diabetes will take place on Friday featuring Suzanne de la Monte, MD, MPH, of the Warren Alpert Medical School of Brown University. In addition, multiple platform sessions throughout the meeting will focus on aging and neurodegenerative diseases including sessions on
Alzheimer’s disease, chronic traumatic encephalopathy, frontotemporal lobar degeneration, Lewy body disease and prion disease. Lastly, this year will also include the first-ever Award for Best Neurodegenerative Disease Case Presented at the 2018 Diagnostic Slide Session.
“We are thrilled to be R13 grant recipients,” said current AANP President Elizabeth Cochran, MD. “Thank you to everyone who dedicated time and focus in developing our proposal, and thank you to the National Institute on Aging for their support.”
Friday, May 4, 2018
Dr. R. Ross Reichard and Dr. Daniel J. Brat will be giving the What Every Neuropathologist Needs to Know lectures at upcoming annual AANP meeting
The 94th
Annual Meeting of the American Association of Neuropathologists will take place June 7-10 in Louisville, Kentucky. On June 9th, Dr. R. Ross Reichard
and Dr. Daniel J. Brat who will be giving the What Every Neuropathologist
Needs to Know lectures. Dr. Reichard will discuss ways a neuropathologist may be involved in legal proceedings. Dr. Brat will talk about the Consortium to Inform Molecular and Practical Approaches to CNS Tumor Taxonomy - Not Official WHO (cIMPACT-NOW), an initiative to address grading challenges in CNS tumors given new findings regarding the impact of molecular signatures on prognosis.
Wednesday, May 2, 2018
Pilomyxoid astrocytoma
 |
| Angiocentricity, a hallmark of pilomyxoid astroctyoma, is demonstrated here |
Subscribe to:
Posts (Atom)
Neuropathology Blog is Signing Off
Neuropathology Blog has run its course. It's been a fantastic experience authoring this blog over many years. The blog has been a source...
-
Neuropathology Blog has run its course. It's been a fantastic experience authoring this blog over many years. The blog has been a source...
-
A neuropathology colleague in Toronto (Dr. Phedias Diamandis) is developing some amazing AI-based tools for pathology and academia. He hel...