The Diagnostic Slide Session at the recent American Association of Neuropathologists annual meeting in Philadelphia featured a fascinating case by Dr. Sandra Camelo-Piragua, Ronald A. Goerss, and David N. Louis of Massachusetts General Hospital. The case was that of a 38-year-old AIDS patient who had been only intermittently compliant with his HAART therapy. He presented to the hospital with seizures in 2009 after a year of fluctuating neurological symptoms. Imaging studies showed the following white matter changes:
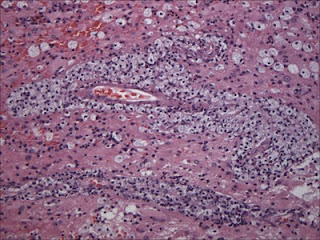
Biopsy showed a marked lymphocytic infiltrate, which included diffuse, perivascular, and follicular arrangements:
The following stains for organisms were all NEGATIVE: AFB, GMS, HSV1, HSV2, CMV, HHV8, and toxoplasma. An H&E/LFB stain demonstrated that this was a leukoencephalopathic process:
Immunohistochemistry of one of the lymphoid follicles indicated that the lymphoid infiltrate was a reactive, rather a neoplastic process:
Polyoma virus immunohistochemistry for the SV40 (a surrogate marker for JC virus due to cross-reactivity) was found to be positive:
So, the final diagnosis rendered was Progressive Multifocal Leukoencephalopathy (PML) with concomitant Immune Reconstitution Inflammatory Syndrome (IRIS). IRIS is an inflammatory response in HIV-infected individuals upon initiation of HAART therapy. The immune response can be so robust as to cause morbidity, particularly with the brain is involved. Thanks to Dr. Camelo-Piragua for providing the images associated with this interesting case, and I wish her the best of luck in her upcoming move to Ann Arbor where she will take a position on the faculty at the University of Michigan!







1 comment:
A new free online CME by Johns Hopkins University School of Medicine is being directed towards pathologists who have patients affected by non-small-cell lung cancer (NSCLC). The online activity is free and will consist of 4 different activities.
Each activity will present different case scenarios using the latest treatment options and diagnostic markers to help pathologists improve patient outcomes.
To learn more about this free online CME activity from Johns Hopkins University School of Medicine, and how you as a pathologist can get up-to-date information on the diagnosis and management of patients with NSCLC please visit: http://www.jhasim1.com/2010-14/index1.aspx .
Post a Comment